
Based on your case, medical history and the surgical decision taken by your surgeon, one of the following operations may be performed:
The gastric sleeve
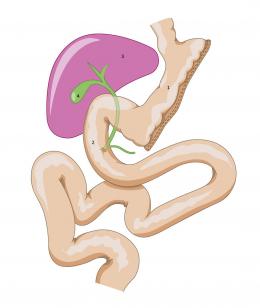
This operation involves removing 80% of the stomach by vertically stapling the organ. This is a feature of surgery referred to as “restrictive” used for the purpose of reducing the quantity of food absorbed by creating a smaller stomach. The cavity can accept only a small quantity of food, so that a sensation of fullness is more rapidly achieved. The remaining absorption takes place as normal. At the same time, the patient will learn how to eat differently.
He will be on a strict diet that calls for self-discipline:
- Meals divided into smaller portions;
- Elimination of high-calorie carbonated drinks as far as possible;
- Acquiring the habit of fluid intake between meals.
This technique is a valid alternative to a gastric bypass. It can also be performed if the gastric ring fails.
The gastric bypass
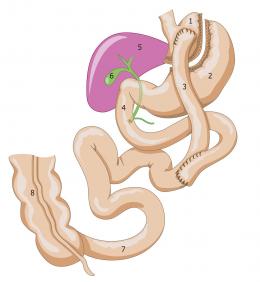
This technique reduces stomach capacity associated with jejunal diversion. It is both an operation that is both restrictive and unfavourable to absorption. By combining these two surgical techniques, digestion is effected in such a way that food is insufficiently absorbed or ‘badly absorbed’. It is combined with a restrictive procedure, thereby helping to limit caloric uptake and achieve greater weight loss.
This operation consists in stapling together a small gastric pocket in order to reduce the size of the stomach and limit the amount of food that can enter. Next, the surgeon turns back a portion of the small intestine to make it extract fewer calories from food (especially fats).
The indications for this operation are a BMI of ≥ 40 and in cases where a gastric ring fails.
Regular monitoring by a cross-disciplinary team is compulsory. Average weight loss also corresponds to a loss of 70% to 100% of excess weight after 12 to 16 months and could be maintained at between 60 to 80% after 5 years.
A vitamin supplement is usually a requirement for life.
Retain : The gastric sleeve and the gastric bypass are currently the 2 most commonly practised techniques.
The mini-bypass
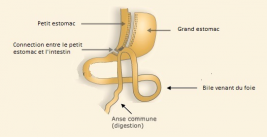
The mini-bypass is a simpler operation than the conventional bypass (a single connection). The operation is easier to reverse. In terms of weight loss, the results are comparable to the standard bypass. The eating comfort level is correct; however, there is less regression in the results over the long term.
The adjustable ring
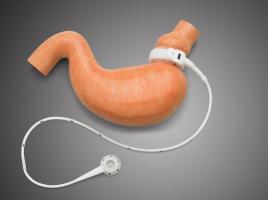
The LASGB (Laparoscopic Adjustable Silicone Gastric Band) was first employed in 1993 and is used to perform restrictive gastric banding: its purpose is to limit the amount of food that can be absorbed.
The assembly works like an hourglass: the food bolus is determined by the volume of the Pavlov stomach and the speed of gastric emptying is slowed down due to the narrowness of the passage. The ring can be adjusted through a subcutaneous or intramuscular cavity implanted in the abdominal wall.
The diameter of the narrow opening can be regulated according to weight loss. The alteration can be made under local anaesthesia or by ultrasound guidance and is performed by a surgeon attended by a radiologist. This adjustment takes no more than 10 minutes.
The indications for the procedure are a BMI of ≥ 40 or ≥ 35 if there are comorbidity factors.
It has the advantage of being reversible.
In the first year, the patient attends a consultation every 2 to 3 months for a follow-up on his weight loss and adjustment of the ring diameter, if necessary. At the end of this period, weight loss achieved should be 30% of the starting weight (a loss of 10 BMI units).
This operation is not used for controlling eating disorders. Ideally, the patient should continue with surgical follow-up (diameter adjustment) and nutritional monitoring.
This technique exposes to the risk of gastro-oesophageal reflux and is being used less and less. it has a long-term success rate of 50%.
